Chronic pain requires an integrated approach and therefore a multidisciplinary treatment method. Clear, non-free agreements between healthcare professionals and other stakeholders such as patients, health insurers, the government are essential. This should not only be about the content of care for patients with chronic pain but also how the care is organized.
An unambiguous definition of chronic pain is difficult to give. The definition of pain as used by the International Association for the Study of Pain (IASP 1994) reads:
Pain is an unpleasant, sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage.
How DAVID plays a significant role in treating patients with Chronic Pain
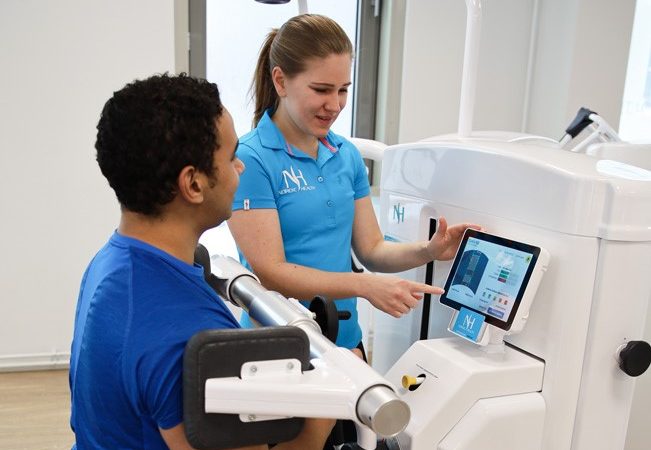
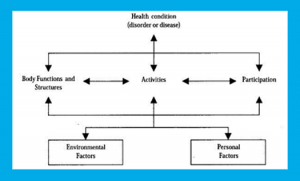
Many clinics that utilize the DAVID Concept treat patients with chronic pain. In countries like the Netherlands and Belgium, integral pain care is an accepted method and is reimbursed by health insurance. During the analysis and physical examination, an inventory is made of the symptoms. The therapeutic analysis also takes place in all dimensions of the ICF model.
Patient-Related Outcome Measurements (PROMs) as part of the digital workflow.
Evidence shows that the systematic use of information from PROMs leads to better communication and decision making between doctors and patients and improves patient satisfaction with care. There is also evidence that patients report better outcomes—for example, improvement in depression. (resource links: 1/2/3/4/5)
However, research on attempts to embed measurement of patient-reported outcomes into routine practice has revealed many technical, social, cultural, legal, and logistical barriers to successful adoption. Patients generally welcome systems that routinely use PROMs. However, they say that patient reporting systems must be used well and not misdirect the focus of the clinical encounter, burden patients, or only focus on factors that have value to clinicians. (resource links: 6/7/8/9/10)
How the EVE platform supports the digital workflow within the world of rehabilitation.
In the USA, standard patient-reported outcome measures are being used to track the outcomes of patients with common surgical conditions. In the Netherlands, Belgium, and Germany, care teams are using web-based EVE applications and E-health to monitor people with chronic pain and provide an individualized approach to rehabilitation treatment.
A holistic approach demands Cognitive Behavior Therapy.
Part of this multidisciplinary approach is the use of cognitive-behavioral therapy. In patients with persistent pain, cognitive behavioral therapy has a positive effect on the acceptance of the pain, the psychological consequences of the pain, the degree of activity, and self-reliance. A chronic pain patient’s progress should be supported with active discussion and psychological support. This holistic approach to treating chronic pain provides long-term benefits for the patients including more confidence and an improved quality of life.

Measurable Success in Exercise Therapy
In order to understand how the DAVID Spine Concept can help chronic pain patients, a primary data analysis was done. An important factor of the therapy is the activation of patients with chronic pain. The DAVID Concept is based on an extensive analysis of the mobility and strength of cervical, lumbar and thoracic spine. This testing is done in the beginning of the treatment program and measured again after 6 (T1) and 12 weeks (T2). A first outcome analysis was done using the David Spine Concept with a total of 609 patients. In summary, the results show significant improvements in patients’ back mobility and strength. Patient-reported pain scores also decreased.
Improvements are clear in measured testing results.
The graph below shows how mobility increases across a range of spinal movements. In 12 weeks, the average improvements range from 9 to 19% increase in mobility.

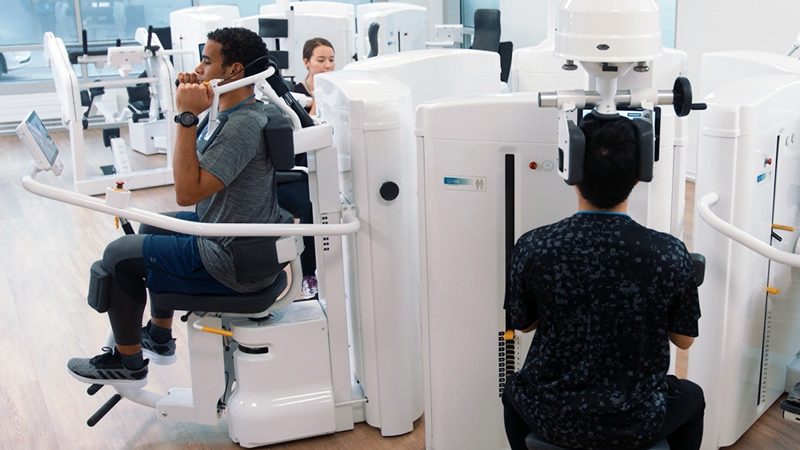
An important part of the therapy is the activation of patients with a long history of pain symptoms. In many of these cases, movement is altogether avoided and psychological factors affect the patient’s desire to move and be active. The DAVID devices provide a safe outlet for the patient to activate the body gradually. The patient has a feeling of regaining control over his/her own body.
The DAVID devices provide a safe outlet for the patient to activate the body gradually.
The graph below provides an understanding of how back strength improves over a 12-week treatment program. Again, there is significant improvement ranging from 25% to 63% across several spinal movements.
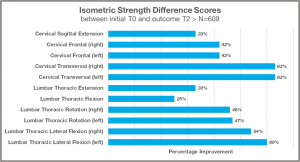
Patients report less chronic pain and better pain management.
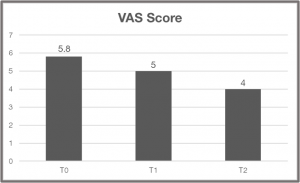
In general, we can say that pain scores are going down. This can be determined from the VAS Score which was collected during the testing sessions. The focus of the multidisciplinary program is not only to reduce the pain scores but to promote load capacity and ADL.
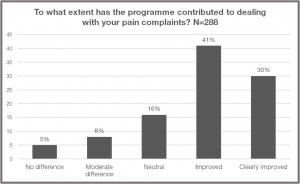
At the end of the 12-week session, the patients were asked “To what extent has the programme contributed to dealing with your pain complaints?” These results indicate that not only the reduction of pain is paramount in the treatment of chronic patients, but that a holistic approach to all aspects of daily life promotes an improved quality of life.
Conclusions:
In the above mentioned patient population, there is a significant increase of strength and mobility after 12 weeks of exercise therapy training. This highlights a promising opportunity for treating chronic pain patients. Nevertheless, in order to determine the effectiveness of the multidisciplinary intervention in chronic pain patients, more research will be needed in the future.

Looking to the future
Emerging information and communication technologies spur the development of new systems designed to capture and use the patient’s voice and feedback. However, the extent to which these systems can improve care will depend on how effectively clinicians respond to the patient feedback.
Future systems for incorporating the patient voice and patient-reported outcomes into office practice need to be based on fundamental principles of patient-centered care such as the timely explanation of information based on patient need and delivery of the information in a way that can help patients take effective actions to protect their health and well-being.
Information and contact.
Would you like more information about the possibilities of DAVID within your medical center, physical therapist practice or rehabilitation setting? Please contact us.
Resources
1) Chen J, Ou L, Hollis SJ. A systematic review of the impact of routine collection of patient-reported outcome measures on patients, providers and health organizations in an oncologic setting. BMC Health Serv Res2013;13:211.
2) Marshall S, Haywood K, Fitzpatrick R. Impact of patient-reported outcome measures on routine practice: a structured review. J Eval Clin Pract2006;12:559-68.
3) Santana M-J, Feeny D. Framework to assess the effects of using patient-reported outcome measures in chronic care management. Qual Life Res2014;23:1505-13.
4) Valderas JM, Kotzeva A, Espallargues M, Guyatt G, Ferrans CE, Halyard MD, et al. The impact of measuring patient-reported outcomes in clinical practice: a systematic review of the literature. Qual Life Res2008;17:179-93
5) Wasson JH, Stukel TA, Weiss JE, Hays RD, Jette AM, Nelson EC. A randomized trial of using patient self-assessment data to improve community practices. Effect Clin Pract1999;2:1-10.
6) Dawson J, Doll H, Fitzpatrick R, Jenkins C, Carr AJ. The routine use of patient-reported outcome measures in healthcare settings. BMJ2010;340:c186
7) Nelson EC, Fisher ES, Weinstein JN. A perspective on patient-centric, feed-forward “collaboratories.” In: Institute of Medicine. Engineering a learning healthcare system: a look at the future: workshop summary. National Academies Press, 2011:149-70.
8) Nelson EC, Hvitfeldt H, Reed R, Grossman D, Lindblad S, Mastanduno M, et al. Using patient-reported information to improve health outcomes and health care value: case studies from Dartmouth, Karolinska and Group Health. 2012.
9) Pincus T, Summey JA, Soraci SA, Jr, Walston K, Hummon N. Assessment of patient satisfaction in activities of daily living using a modified Stanford Health Assessment Questionnaire. Arthritis Rheum 1983;26:1346-53
10) Taylor W, Wang MC, Lozano P, Bradford SC. Patient-reported data to engage patients and inform clinical and population care: using patient-reported outcome data to provide patient-centered care and improve clinical care delivery. National Quality Conference, Sacramento, CA, 4 June 2013.
Bastiaan Meijer
Digital Marketing Manager
bastiaan.meijer@davidhealth.com
 English
English